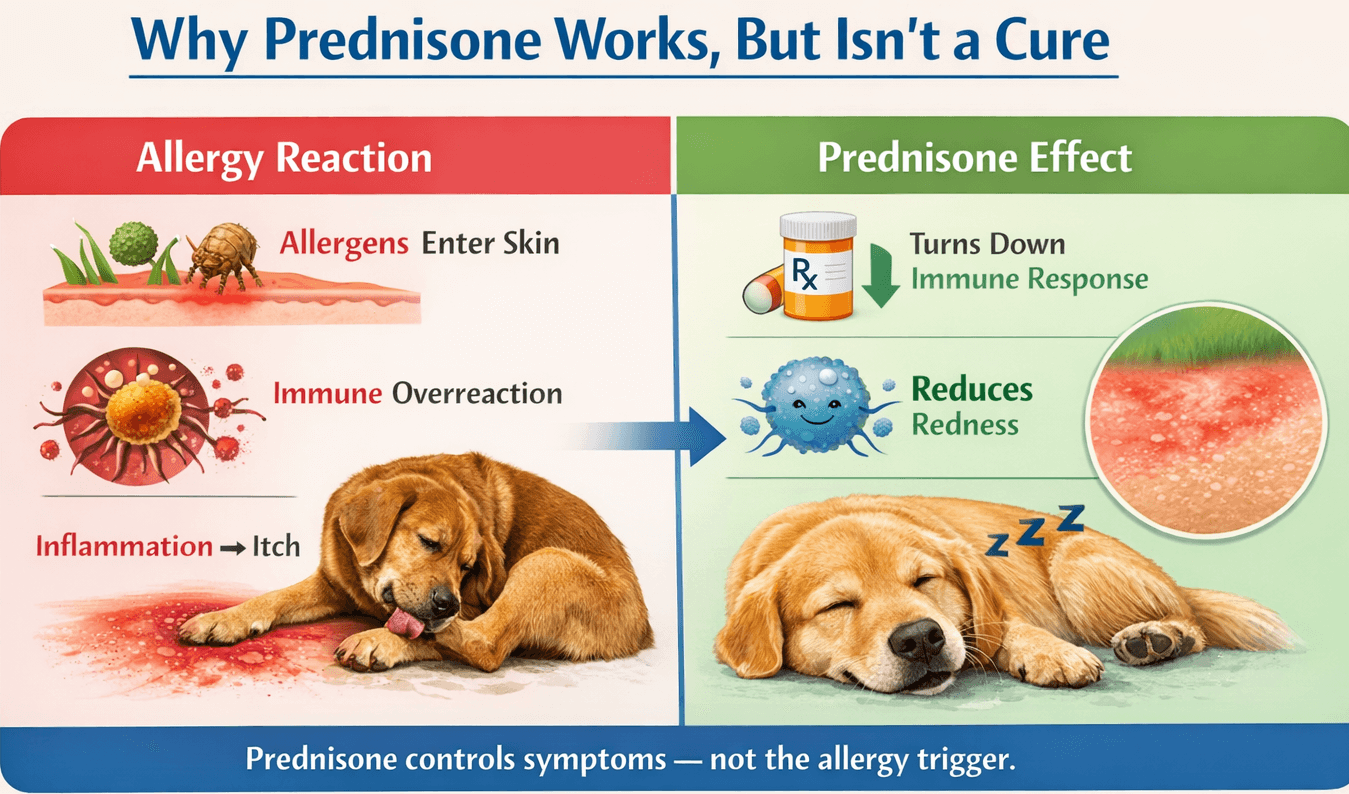
How Long Can a Dog Stay on Prednisone for Allergies? Vet Explains
Most dogs receive prednisone safely for short periods such as 2–4 weeks, while longer use depends on dose, monitoring, and whether additional allergy treatments are introduced to reduce steroid reliance.
🐾 In This Guide:
Dog prednisone is a critical subject for pet parents managing dog allergies. When a dog can’t stop scratching despite baths, supplements, and environmental changes, prednisone is often considered.
Prednisone offers profound relief, but it also presents trade-offs. The medication suppresses inflammation broadly, helping control allergic symptoms without addressing the underlying trigger. Chronic allergies in dogs are long-term diseases that typically require ongoing management rather than a single medication solution. Many allergy dogs first show subtle signs like ear irritation or paw licking before more severe flare-ups develop.
Modern veterinary allergy care focuses on reducing flare frequency while minimizing long-term steroid exposure through multimodal treatment strategies outlined in the AAHA Management of Allergic Skin Diseases Guidelines, which closely reflect how veterinarians, like myself, manage chronic allergy patients in everyday clinical practice.
The central question isn’t whether prednisone works as it often works dramatically. The real question is about long-term use:
How long can a dog be on prednisone for allergies safely?
The answer depends on the prednisone dosage and frequency, monitoring (especially blood work), your individual dog’s medical condition(s), and whether prednisone is being used as a bridge to other treatment options or as a long-term treatment plan. This is why it is important to have a working relationship with your vet for the best treatment options.
Short-Term vs. Long-Term Use of Prednisone for Dog Allergies: What’s the Difference?
Prednisone can be used safely in both short-term and longer treatment plans, but the goals and management strategy differ.
Short-Term Prednisone Use (Typically 2–4 Weeks)
Short courses of prednisone are commonly used in emergency allergy management or severe flare-ups. When seasonal allergens or sudden exposures trigger intense itching, prednisone acts like hitting “mute” on inflammation long enough for the skin to heal. Recurring inflammation or warmth in the ears can signal ongoing allergic disease activity.
Recent clinical research evaluating dogs receiving short anti-inflammatory courses of prednisone found that behavioral or physical changes such as increased thirst, appetite, panting, or urination were reported in the majority of dogs within the first two weeks of treatment, even at standard dosing levels. While these effects are usually temporary, they highlight why veterinarians prepare pet parents for noticeable changes early in therapy.
Short-term treatment is often used to:
Control severe itch or allergic crisis
Interrupt the itch–scratch–infection cycle
Persistent paw licking is often one of the earliest signs this cycle has begun.
Allow damaged skin to recover
Bridge your dog onto longer-term allergy strategies
Most dogs experience predictable and manageable side effects, and treatment typically includes:
Daily dosing for a limited period
A planned taper (gradual dose reduction)
A goal of discontinuation once the flare is controlled
Long-Term Prednisone Use (Generally Beyond 4–6 Weeks)
Long-term therapy requires a different mindset focused on risk management rather than rapid symptom control.
For some dogs with chronic environmental allergies, treatment may become seasonal or ongoing when other therapies alone are insufficient.
Long-term prednisone plans typically aim for:
The minimum effective dose
Lower dosing or alternate-day therapy
Regular veterinary rechecks and blood work
Continuous monitoring for side effects and flare patterns
Current veterinary dermatology guidelines emphasize that allergic skin disease is best managed using a multimodal approach rather than relying on a single medication such as prednisone. The AAHA Management of Allergic Skin Diseases Guidelines outline step-by-step strategies veterinarians use to reduce flare frequency and improve long-term quality of life.
What Matters More Than Time on Prednisone
In veterinary medicine, “long-term” does not refer to a single fixed duration. What matters most is how prednisone is used over time:
High daily doses vs. low maintenance doses
Continuous use vs. strategic seasonal courses
Active monitoring vs. unchanged long-term therapy
Not every dog requires lifelong steroids. Allergy testing, symptom tracking, and close collaboration with your veterinarian often reveal patterns that allow targeted or seasonal treatment, significantly reducing total lifetime steroid exposure.
Tracking when itching worsens, such as seasonal changes, nighttime flares, grooming, or environmental exposure, helps us safely reduce steroid reliance over time.
👉 If you want a simple way to track these patterns at home, you can download my free Itch Tracker here.
If your dog needs repeated rounds of prednisone, tracking patterns can help your vet make more informed decisions over time. HotSpotter is a veterinary professional-created pet allergy tracker that helps you log itch scores, photos, flare-ups, treatments, and possible triggers in one place, so your vet has a clearer timeline rather than relying on memory alone.
How Prednisone Works for Dog Allergies: The Science Behind the Relief
Prednisone is a glucocorticoid that reduces inflammation by altering the behavior of immune cells. When allergies trigger inflammation, the immune system releases mediators that cause itching, redness, and swelling. Prednisone suppresses this immune response and decreases the inflammatory cascade.
Prednisone is converted to prednisolone in the liver and then binds to glucocorticoid receptors throughout the dog’s body. This binding reduces the levels of inflammatory chemicals such as cytokines and prostaglandins.
What pet parents often notice first:
Less itching within 24-48 hours
Improved sleep
Less chewing/licking/scratching
Reduced redness and swelling
Because prednisone works broadly, it can often relieve symptoms faster than many other allergy therapies. But that same “broad suppression” is why long-term prednisone use carries more risk.
In clinical practice, prednisone is often started at anti-inflammatory doses and then tapered to the lowest effective dose once symptoms improve, rather than continued indefinitely as a sole therapy.
Prednisone Dosage for Dogs: Why Your Vet Calculates It Individually
Prednisone dosing in dogs is based on body weight, the reason it is being prescribed, the severity of symptoms, other medications your dog is taking, and your dog’s overall health.
For allergy flares, veterinarians, like myself, often use prednisone at an anti-inflammatory dose for a short period of time, then taper down once symptoms are more controlled. Higher immunosuppressive doses may be used for certain severe conditions, but these carry a greater risk of side effects and are not typically the goal for routine allergy management.
This is why two dogs of the same size may receive different prednisone plans. One dog may need a short taper for an acute flare, while another may need a broader allergy plan that includes infection control, flea prevention, topical therapy, guidance on diet trials, or long-term allergy medication.
Important: Never start, stop, increase, decrease, or restart prednisone without your veterinarian’s guidance. Even small changes can affect the tapering schedule and may increase the risk of side effects or rebound symptoms.
For chronic allergies, the goal is usually the lowest effective dose for the shortest reasonable time while working toward a safer long-term plan.
Most Common Side Effects of Prednisone in Dogs
Short-term courses commonly cause a predictable set of changes. These are the most common side effects of prednisone in dogs:
Increased thirst
Increased urination (often more overnight bathroom breaks)
Increased appetite
Panting
Restlessness or “wired” behavior
These effects are dose-dependent: dogs on high doses typically show more pronounced changes than dogs on lower doses or alternate-day therapy.
Possible Side Effects With Long-Term Prednisone Use
With longer use, the list of possible side effects expands, and some become more clinically meaningful. Potential health issues include:
Weight gain
Muscle weakness and reduced stamina
Thinning skin, fragile skin, and delayed wound healing
Increased susceptibility to infections (skin, ears, urinary tract)
Dogs receiving steroids may also become more prone to secondary ear infections if underlying allergies remain uncontrolled.
Gastrointestinal upset (vomiting/diarrhea, ulcer risk)
Elevated liver enzymes on blood work, such as ALKP
Increased risk of diabetes mellitus
Cushing’s-like changes over time
Cushing’s disease is a hormonal disorder involving excess cortisol exposure, which produces many of the same clinical signs seen with chronic steroid therapy.
Most dogs will not experience every effect, but the risk of significant side effects rises with:
Higher daily dosing
Longer duration
Underlying chronic conditions
Long-Term Risk: Steroid-Induced Cushing’s Disease
One of the concerns with long-term prednisone use is steroid-induced Cushing’s disease, also called iatrogenic hyperadrenocorticism. This happens when a dog’s body is exposed to steroid medication for long enough that it begins to show signs of cortisol excess.
Possible signs include:
Increased thirst and urination that does not improve
Increased appetite and weight gain
Panting, even at rest
Muscle weakness or a pot-bellied appearance
Thin skin, blackheads, or slow wound healing
Hair thinning or hair loss
More frequent skin or urinary infections
This is one reason we try to use prednisone carefully, especially for chronic allergy dogs. If your dog needs repeated steroid courses, it may be time to talk with your vet about longer-term allergy options and monitoring bloodwork.
Never stop prednisone suddenly unless your veterinarian tells you to. Dogs on longer courses often need a gradual taper so their bodies have time to adjust.
Blood Work and Monitoring During Long-Term Prednisone Use
If prednisone is being used beyond a few weeks, monitoring is what keeps long-term treatment responsible.
What your veterinarian may monitor
Weight and body condition
Drinking/urination changes
Skin and ear infection recurrence
Muscle condition
Blood work trends (liver enzymes, glucose, kidney values)
Urinalysis (especially in dogs prone to urinary issues)
A common plan is baseline labs before therapy, then rechecks every 3 - 6 months. This isn’t “extra”, it’s the safety net that allows continued treatment decisions to be made thoughtfully.
Adrenal Glands, Addison’s Disease, and Why Tapering Matters
One of the most important long-term risks of prednisone therapy is adrenal suppression. When prednisone is present, a dog’s adrenal glands reduce their natural cortisol production. This is why long-term steroids generally cannot be stopped suddenly.
Abrupt discontinuation after extended treatment can lead to an adrenal crisis, because the body may temporarily be unable to produce adequate cortisol on its own.
Long-term steroid exposure can also cause Cushing’s-like changes, sometimes called iatrogenic Cushing’s syndrome. These effects occur because the body is exposed to excess steroid hormone from medication rather than producing it naturally. Many of these changes improve once prednisone doses are reduced or discontinued appropriately.
Tapering allows the adrenal glands time to resume normal hormone production safely.
This becomes especially important in dogs with:
Known or suspected Addison’s disease
Other adrenal gland disorders
Prednisone may also be used as replacement therapy in dogs that require steroid hormone support, such as those with Addison’s disease, though these cases are managed differently, but still require close veterinary supervision.
Prednisone Dosage, High Doses vs. Lower Doses, and “How Long Is Too Long?”
There is no single universal safe duration and the biggest driver isn’t just time. It’s cumulative exposure and dose intensity.
A dog on a lower dose every other day may tolerate therapy far longer than a dog on high doses daily.
In real life, veterinarians think in these terms:
Can we taper to the minimum effective dose?
Can we shift to alternate-day dosing?
Can we reduce reliance by adding other treatment options?
Are we seeing adverse reactions or quality-of-life tradeoffs?
If your dog needs prednisone beyond 4 - 6 weeks, it’s a sign to zoom out and reassess the long-term allergy plan (not necessarily panic, but reassess and make sure you are staying in contact with your veterinarian regularly for advice).
Drug Interactions With Prednisone and Other Prescription Drugs
Before your dog starts prednisone, tell your veterinarian about every medication, supplement, flea/tick product, and over-the-counter product your dog receives. Prednisone can interact with other prescription drugs. Some combinations raise the risk of side effects or complications.
Important drug interactions to discuss with your vet
NSAIDs: carprofen (Rimadyl), meloxicam, deracoxib, grapiprant, etc
These should not be combined with prednisone unless your veterinarian specifically directs it, because the combination can increase the risk of stomach or intestinal ulceration and bleeding.
Certain antibiotics or antifungals
Diuretics
Vaccinations
Timing matters Prednisone at immunosuppressive doses can reduce the effectiveness of live vaccines. If your dog is due for vaccines, discuss timing with your vet — in most cases, vaccines are postponed until after the prednisone course is complete.
Insulin (diabetic dogs)
Prednisone raises blood glucose levels, which can destabilize a diabetic dog's insulin requirements significantly. Diabetic dogs on prednisone require very close monitoring and frequent glucose checks.
Other immunosuppressive medications
Always tell your veterinarian what your dog is taking, including supplements, because interactions can influence safety.
Prednisone and Dogs With a Medical Condition: Extra Considerations
Some dogs can take prednisone safely with monitoring, but certain medical conditions require extra caution. Your vet may adjust the plan if your dog has:
Kidney disease
Liver disease
Diabetes mellitus
Recurrent urinary tract infections
Heart disease
Bladder stones
Certain types of cancers
Prednisone may still be used in some of these cases, but the risk/benefit calculation becomes tighter.
Prednisone is also used for other inflammatory conditions, including:
Inflammatory bowel disease
Certain autoimmune diseases
These are situations where long-term treatment may be medically necessary, and monitoring becomes even more important.
Missed Dose, Next Dose, and When to Seek Medical Advice
If you miss a dose, the safest move depends on timing and how long your dog has been on prednisone.
General guidance pet parents are often given:
If you remember soon, give the dose.
If it’s close to the next dose, skip the missed dose.
Don’t double up unless your veterinarian tells you to.
If your dog has been on long-term prednisone, do not abruptly stop without veterinary guidance.
Signs of Prednisone Overdose or Serious Reaction in Dogs
Seek medical advice urgently if you notice:
Collapse or extreme weakness
Repeated vomiting
Black/tarry stool
Severe lethargy
Signs of a serious infection
In an emergency, ASPCA Animal Poison Control Center support can be helpful while you arrange veterinary care (especially if there’s accidental overdose or concerning symptoms).
Conventional Wisdom vs. Reality: Long-Term Prednisone Use
Veterinary teaching around steroids has evolved. Older guidance often discouraged any long-term prednisone use. Clinical reality is more nuanced.
Some dogs tolerate low-dose prednisone for months (or longer) with minimal complications and excellent quality of life improvement. Others develop health issues quickly.
The truth lies in individualization:
continuous daily dosing vs intermittent/strategic dosing
high doses vs lower doses
monitoring and adjustment vs “set it and forget it”
For severe allergies where other options aren’t effective or affordable, prednisone can remain a legitimate choice when careful monitoring is in place.
Managing Dog Allergies Beyond Prednisone: Treatment Options
Prednisone works best as part of a broader allergy plan, not as the entire strategy.
Steroid-sparing treatment options to discuss with your vet
Prescription allergy medications (Apoquel, Cytopoint)
Allergen-specific immunotherapy (often done most effectively with a veterinary dermatology office)
Antihistamines (rarely efficient alone due to variable effectiveness)
Essential fatty acids such as Omegas (skin barrier support and anti-inflammatory effects)
Medicated bathing routines with veterinary recommended active ingredients that support the skin (Often Chlorhexidine, Ophytrium, and/or Phytosphingosine)
Proper ear care becomes especially important in allergy-prone dogs.
Diet trials (for suspected food allergy)
Environmental modification (allergen load reduction)
Long-term allergy control rarely depends on a single medication. Small daily changes in bathing routines, barrier support, and environmental management often reduce flare frequency significantly.
👉 The 28-Day Skin & Itch Reset walks through these step-by-step strategies used in veterinary allergy management.
Tracking Patterns: The Key to Effective Allergy Management
The most powerful long-term tool isn’t another medication. It’s consistent observation.
Tracking helps you answer questions like:
Is your dog worse at night?
Do flares follow grooming, grass walks, or weather changes?
Did symptoms improve after a bath or wipe routine?
Did itch return when medication timing changed?
A simple daily journal can turn reactive care into proactive management. It also helps your veterinarian make better decisions faster.
Tracking patterns such as seasonal flares, nighttime licking, or post-walk itching can dramatically improve treatment decisions.
Limitations and Considerations
Even when prednisone works beautifully, it’s not ideal for every dog or every scenario.
Prednisone may be less suitable when:
a dog needs escalating doses to get relief
the dog has diabetes risk or chronic infections
the dog develops adverse reactions early
owners can’t maintain monitoring (blood work / rechecks)
Prednisone doesn’t change what a dog is allergic to, it only suppresses the reaction. Without addressing triggers, you can end up treating symptoms indefinitely rather than managing the disease.
The easier you make tracking, the more useful it becomes.
HotSpotter was created by veterinary professionals to help pet parents track allergy symptoms, itch scores, photos, treatments, possible triggers, and flare patterns over time. If your dog has needed prednisone more than once, this kind of history can help your vet see what is changing, what is helping, and whether your dog may need a longer-term allergy plan.
Available now on Android and web browser. iPhone app coming soon.
FAQs About Prednisone in Dogs
-
Most dogs receive prednisone safely for short periods such as 2–4 weeks during allergy flare-ups. Longer use may be appropriate in some cases but depends on dose, monitoring, and whether other allergy treatments are introduced to reduce long-term steroid exposure. The best option is to work closely with your veterinarian, who knows your pet’s needs and risks best.
-
Prednisone can be safe when used strategically under veterinary supervision. Many veterinarians use it as a short-term rescue medication or at the lowest effective dose while building a broader allergy management plan. It is up to your veterinarian to determine the safest long-term plan for your pet.
-
Long-term daily prednisone use increases the risk of side effects such as weight gain, infections, muscle weakness, elevated liver enzymes, diabetes, or Cushing’s-like changes. Regular monitoring helps reduce these risks. If you are concerned about these, please reach out to your veterinarian.
-
Long-term steroid therapy can cause iatrogenic Cushing’s syndrome, meaning symptoms occur due to medication exposure rather than a naturally occurring disease. Many changes improve once doses are reduced appropriately. If you are concerned about this, please contact your veterinarian so they can determine if this is a risk for your pet.
-
Prednisone suppresses natural cortisol production by the adrenal glands. Stopping abruptly after extended treatment can lead to an adrenal crisis, which is why veterinarians gradually taper the medication.
-
Many dogs show improvement within 24–48 hours, including reduced scratching, improved sleep, and decreased skin inflammation.
-
Yes. Options may include Apoquel, Cytopoint, allergen immunotherapy, medicated bathing routines, dietary trials, and environmental management strategies designed to reduce flare frequency. The best option for most patients is a multi-modal approach to treat the many symptoms of allergies.
-
Contact your veterinarian ASAP if you notice vomiting, diarrhea, severe lethargy, collapse, black stools, signs of infection, or sudden worsening symptoms. These could all be very serious side effects.
Key Dog Prednisone Takeaways
Prednisone can be extremely effective for allergic itch — but the safest use is strategic and individualized.
Key takeaways for pet parents:
Short-term prednisone (often 2–4 weeks) is commonly used for severe flare-ups and is usually well tolerated.
Long-term prednisone use is sometimes necessary, but it requires monitoring, dose reduction strategies, and a long-term allergy plan.
The most common side effects of prednisone include thirst, urination, appetite increase, panting, and restlessness.
Significant side effects are more likely with high doses and long-term daily treatment.
The biggest “safety” question is not just time — it’s dose, monitoring, and your dog’s medical condition.
Never stop long-term prednisone suddenly; tapering protects the adrenal glands.
Tracking symptoms helps your vet find the lowest effective dose and identify patterns that reduce flare frequency.
You’ve got this, and I’m here to help every step of the way. 🐾
💛 Dr. Fran, DVM, CPEV — veterinarian and founder of Kind Vet Wellness.
Learn more about Dr. Fran → Click Here
Medical Disclaimer:
The content on this website is intended for educational purposes only and does not replace professional veterinary medical advice, diagnosis, or treatment. Always consult your veterinarian regarding your pet’s individual health concerns.